The 3 Stretches That Fixed My Lower Back Pain After 5 Years of Failed Treatments
Five Years of Lower Back Pain — And What Finally Changed Everything
I lived with non-specific lower back pain for five years. Not severe, not disabling — but a persistent ache always present and would flare into genuine pain after long car rides, heavy lifting, or sitting at a desk for more than an hour. I saw a GP, a chiropractor, an orthopaedic specialist, and a physiotherapist. Nothing resolved it permanently.
The breakthrough came from a yoga teacher who watched me move and identified, within ten minutes, that my hip flexors were so shortened from desk work that my pelvis was locked in anterior tilt — meaning my lumbar spine was permanently compressed. Not an injury. Not a disc problem. A flexibility problem that years of treatment had circled around without identifying.
Three specific stretches performed every morning for 8 weeks resolved pain that five years of treatment had only temporarily managed. This article shares those stretches, explains the mechanism, and provides the daily routine that has kept my lower back pain-free for three years since.
Why Most Lower Back Pain Isn’t Actually a Back Problem
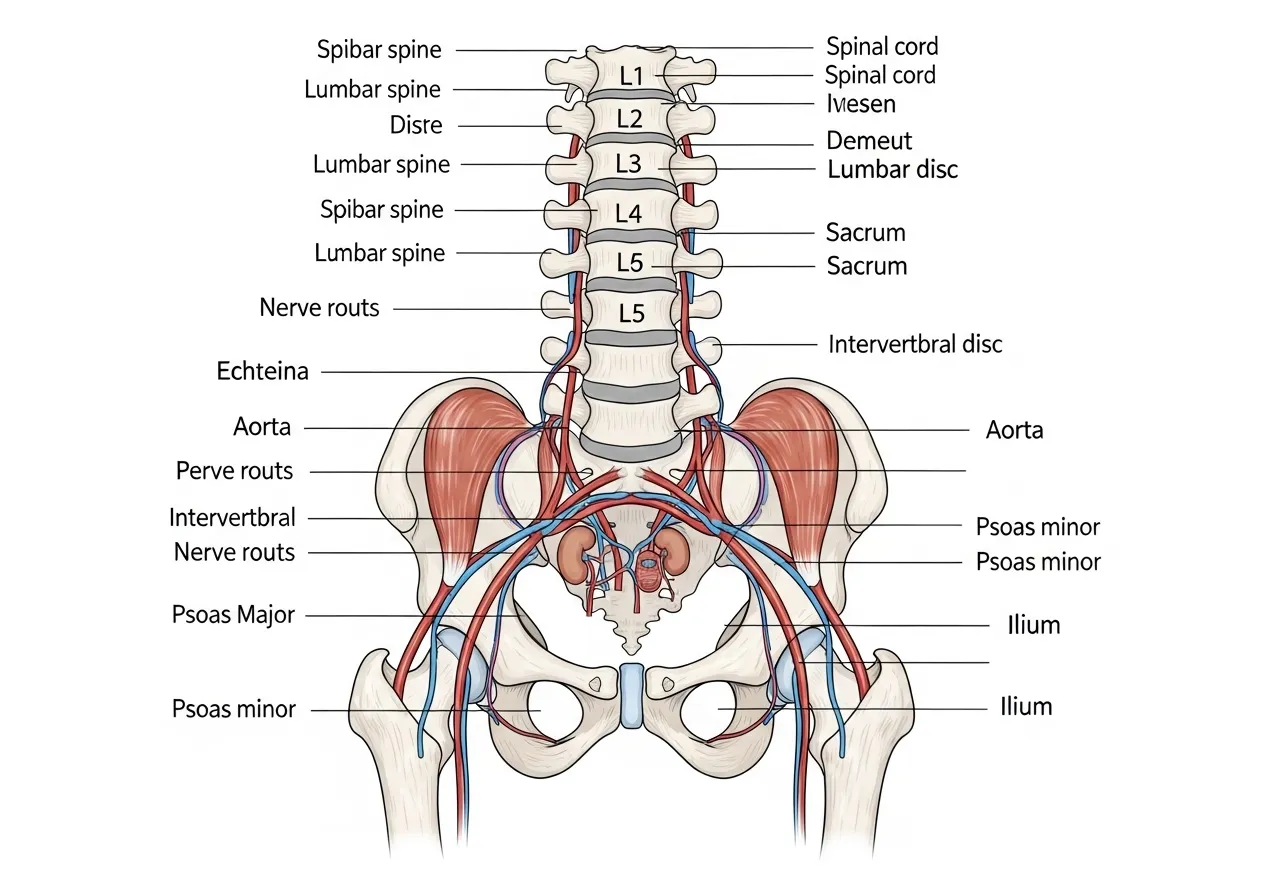
Research on non-specific lower back pain consistently identifies hip flexor tightness, piriformis tension, and poor lumbopelvic mobility as primary contributing factors rather than the lumbar spine itself being the source. The mechanism: tight hip flexors (particularly the psoas major) pull the lumbar vertebrae forward into excessive lordosis, compressing the lumbar facet joints and posterior disc spaces. The psoas, with proximal attachment on the lumbar vertebrae, creates direct compressive force on the lumbar spine when shortened — estimated at approximately 100N of compression just from resting psoas tone in people with significant tightness.
The Role of the Piriformis
The piriformis is a small external rotator of the hip that, when tight, compresses the sciatic nerve and creates direct tension on the sacroiliac joint. Many people experiencing “lower back pain” are actually experiencing referred pain from piriformis tightness — producing symptoms that feel like lumbar pain but originate from a muscle that can be addressed with a single specific stretch.
Addressing the Source, Not the Symptom
Years of treating the location of pain (the lower back) without addressing the source (hip flexor and piriformis restriction) produces the temporary-improvement cycle most lower back pain sufferers experience. Addressing the mechanical cause directly — through the three stretches that follow — produces lasting change rather than temporary symptom management.

The Three Stretches: Complete Technique Guide
Stretch 1: Kneeling Hip Flexor Stretch (Lunge Stretch)
Kneel on your left knee with right foot forward in a half-kneeling position. The critical element: tuck your pelvis posteriorly — squeeze the left glute and tuck the tailbone under, eliminating the anterior tilt. Without this pelvic tuck, the stretch reaches the hip flexors only partially. Gently shift your hips forward until you feel a deep stretch in the front of the left hip and groin. Hold for 60-90 seconds per side. Repeat twice on each side. Total: approximately 6 minutes.
This stretch directly lengthens the psoas and iliacus — the hip flexors most responsible for anterior pelvic tilt and lumbar compression. The kneeling position fixes the hip’s attachment point, ensuring the stretch targets the hip flexor rather than the lumbar spine. Research on hip flexor stretching and lower back pain consistently identifies hip flexor flexibility as a modifiable factor in non-specific lower back pain.
Stretch 2: Supine Piriformis Stretch (Figure Four)
Lie on your back with both knees bent, feet flat on the floor. Cross your right ankle over your left knee, creating a figure four. Flex the right foot (toes toward shin) to protect the knee. Gently pull the left knee toward your chest — you will feel a deep stretch in the right glute and outer hip. Hold 60 seconds per side, twice each. If you cannot reach your left leg, loop a towel or strap around it.
The figure-four stretch targets the piriformis specifically and can produce immediate relief in people with piriformis-sourced symptoms. The simultaneous sciatic nerve decompression that occurs as the piriformis releases is why many people feel almost immediate relief in what they had been describing as “lower back pain” after performing this stretch.
Stretch 3: Child’s Pose with Lateral Shift
From kneeling, sit hips back toward heels and reach both arms forward, dropping the chest toward the ground. For the lateral shift: walk both hands 15-20 cm to the right (30 seconds), then to the left (30 seconds). Hold 60 seconds center, 30 seconds each side, two rounds. Total: approximately 3 minutes.
Child’s pose creates gentle lumbar flexion that decompresses the posterior elements of the lumbar spine — the facet joints and posterior discs that anterior tilt compresses. The sustained gentle traction creates a neuromodulatory effect that directly reduces pain signals from compressed structures.

The Science of Why Daily Practice Produces Lasting Results
Neurological vs. Structural Change
The immediate improvement in range of motion from a single stretch session is primarily neurological — the nervous system’s stretch tolerance temporarily increases. This is why a single session provides short-term relief but the problem returns: structural changes in muscle and connective tissue length that produce lasting flexibility improvement require 6-8 weeks of daily practice. Consistent daily stretching of 60-90 second holds produces both neurological adaptation and structural tissue lengthening — the neurological changes are temporary; the structural changes are permanent.
Central Sensitization and Chronic Pain
Chronic lower back pain involves not just mechanical factors but central sensitization — the nervous system’s amplification of pain signals after prolonged exposure. Daily mobility practices produce a counter-stimulus to this sensitization: the pleasant sensation of stretching and improved movement freedom provide positive neural inputs that gradually reduce pain amplification. This neurological component explains why daily practice produces faster resolution than weekly sessions even when total stretching time is equivalent.
Why the Morning Is Optimal
Morning stretching targets the period when compression and stiffness are at their peak — the lumbar discs rehydrate and expand during sleep, creating the morning stiffness most lower back pain sufferers experience on waking. Performing the routine before getting up or immediately after significantly reduces this morning pain signature and sets the mobility baseline for the rest of the day. Research on flexibility interventions and lower back pain supports stretching as an evidence-based component of non-specific lower back pain management.

Building the Daily 10-Minute Routine
The Complete Morning Sequence
Knees to chest gentle pull (1 minute): lying on back, pull both knees gently toward chest, rock gently side to side to mobilize the sacroiliac joint. Kneeling hip flexor stretch (4 minutes: 2 rounds × 60 seconds each side). Figure-four piriformis stretch (4 minutes: 2 rounds × 60 seconds each side). Child’s pose with lateral shift (1 minute: 30 seconds center, 15 seconds each side). Total: 10 minutes. Performed daily without exception.
Habit Stacking for Consistency
The single biggest obstacle to stretching’s effectiveness is consistency. Attach the routine to an existing morning habit — before coffee, after showering, during the first 10 minutes of the day. I perform the routine while my coffee brews — it takes almost exactly the same time, and I’ve never needed willpower to start because starting is the same as starting coffee. This habit stacking makes the routine invisible rather than a separate commitment.
When to Expect Results
Most people report noticeable improvement within 2-3 weeks of daily practice. Significant reduction in baseline pain typically takes 6-8 weeks. Complete resolution in cases where flexibility deficits are the primary cause takes 3-6 months of consistent practice. The milestone that matters most: when the back stops being the first thing you’re aware of on waking.
Addressing the Source: Sitting Less
The stretches address hip flexor shortening; reducing the hours of hip flexion that create it prevents the problem from rebuilding daily. Standing desks, hourly movement breaks (2 minutes of standing per hour of sitting), and replacing some sitting time with floor sitting (hip-opening positions) all reduce the accumulation that daily stretching is working against.

Beyond Stretching: The Complete Lower Back Health Approach
Core Stability: The Essential Complement
Hip flexor stretching removes one source of lumbar loading; core stability prevents the lumbar spine from moving excessively under that reduced load. Dead bugs, bird dogs, and planks — exercises training anti-extension and anti-rotation core function — complement the flexibility work by building the muscle support that holds the improved lumbar position. Without the strengthening component, flexibility gains allow more movement but don’t provide the structural support that prevents pain under load.
Glute Strengthening
Weak glutes are frequently a companion to tight hip flexors — the inhibited gluteal muscles fail to produce adequate hip extension, forcing the hamstrings and lower back to compensate. Adding glute bridges, hip thrusts, and single-leg deadlifts to the routine alongside the stretches addresses both sides of the hip complex simultaneously, accelerating lower back pain resolution significantly compared to stretching alone.
Should I stretch if my back is in acute pain? Gentle movement (child’s pose, knees-to-chest) is generally appropriate during acute lower back pain. Avoid deep hip flexor stretching during acute flare-ups — this can increase pain if lumbar muscles are in protective spasm. Consult a healthcare provider for acute pain that is severe, involves leg symptoms, or follows an injury.
How long should I hold each stretch? Research indicates holds of 60-90 seconds produce greater flexibility improvements than 15-30 second holds. The neurological habituation that allows muscle release requires sustained time at end range — shorter holds produce only temporary neurological changes without structural tissue adaptation.
Can stretching make lower back pain worse? Some types — particularly disc herniations producing sciatica — can be aggravated by certain stretches. The figure-four stretch can increase sciatica symptoms in people with lateral disc protrusion. If any stretch consistently produces pain radiating into the leg, stop that specific stretch and consult a physiotherapist for modified alternatives.
Is yoga better than targeted stretching? Research supports both yoga and targeted stretching for chronic lower back pain. The advantage of targeted stretching is specificity and time efficiency. The advantage of yoga is the additional guidance, community, and comprehensive movement practice. A targeted daily routine plus occasional yoga classes captures benefits of both.
How is this different from physiotherapy? The stretches described here align with exercises commonly prescribed in physiotherapy for non-specific lower back pain from hip flexor and piriformis tightness. A physiotherapist provides individualized assessment that may require different interventions. If lower back pain persists beyond 6-8 weeks of consistent self-management, professional evaluation is warranted — these stretches are a starting point and adjunct, not a substitute for that evaluation.












