Ankle Mobility: The Hidden Problem Behind Your Squat, Running, and Knee Pain

The Joint Your Entire Fitness Life Depends On Without You Knowing It
I had been squatting for four years before anyone mentioned ankle mobility to me. My squat depth was limited, my heels occasionally lifted at the bottom, and I had a persistent anterior knee discomfort that physiotherapy kept temporarily resolving without eliminating. The physio who finally identified the cause spent thirty seconds measuring my ankle dorsiflexion, looked up, and said: “Your ankles are the problem.”
Restricted ankle dorsiflexion — the ability to bring the shin toward the foot — was limiting my squat depth, causing compensatory forward lean that overloaded my knees, and forcing every step of my running to land with different mechanics than optimal. Six weeks of daily ankle mobility work changed my squat, reduced my knee discomfort, and measurably improved my running economy. The ankle was the upstream cause of problems I had been treating downstream for years.
Ankle mobility is the most overlooked joint in fitness training and the one with the widest-reaching consequences for everything else. This guide explains what ankle dorsiflexion is, how to measure it, and the specific exercises that restore it — with the precision that produces actual change rather than temporary improvement.
What Ankle Dorsiflexion Actually Is
Ankle dorsiflexion is the movement of bringing the top of the foot toward the shin — the opposite of pointing the toes. During the squat descent, running ground contact, and stair climbing, the ankle must dorsiflex to allow the knee to travel forward over the toes. When dorsiflexion is restricted, the ankle reaches its range of motion limit before the movement is complete, forcing compensations: heels rise, knees track inward, the torso leans forward excessively, or the movement is simply cut short.
Why Modern Life Restricts Ankle Mobility
Elevated heel footwear — even modest heel-to-toe drop in standard athletic shoes — maintains the calf and Achilles complex in a shortened position throughout the day. Over months and years, the calf muscles, Achilles tendon, and posterior ankle capsule adaptively shorten to match the position they spend most time in. Sedentary sitting reduces the ankle’s habitual range of motion usage. Previous ankle sprains — which most active adults have experienced at least once — create capsular scarring that mechanically restricts the joint range of motion beyond what calf tightness alone explains.
The Anatomy of Ankle Dorsiflexion: Why This Range of Motion Controls Everything
Ankle dorsiflexion — the movement of pulling the foot toward the shin — is controlled by the flexibility of the calf muscles (gastrocnemius and soleus), the Achilles tendon, and the posterior ankle joint capsule. When any of these structures is tight, the ankle cannot dorsiflex sufficiently, and the body compensates through adjacent joints: the heel rises, the knee caves inward, or the hip rotates externally to create the appearance of the required range of motion while actually avoiding the ankle movement. These compensations are biomechanical compromises that distribute load to structures not designed to bear it repeatedly under training loads. The gastrocnemius crosses both the ankle and the knee, meaning it is stretched most effectively when the knee is straight. The soleus crosses only the ankle, meaning it is the primary restrictor when the knee is bent (as in the bottom of a squat). Both must be adequately flexible for complete functional ankle dorsiflexion. The posterior capsule — the ligamentous structure at the back of the ankle joint — can become restricted after ankle sprains or simply from chronic tightness, requiring joint mobilization rather than muscle stretching for improvement. Understanding which structure is limiting is essential for selecting the correct intervention. Research on ankle dorsiflexion and lower extremity injury confirms that restricted ankle dorsiflexion is associated with significantly increased injury risk in running, jumping, and squatting activities.
How Ankle Mobility Affects Every Major Lower Body Exercise
The ankle’s influence extends beyond the squat to affect virtually every lower body exercise and athletic movement. In the deadlift, insufficient ankle dorsiflexion causes the lifter to shift weight forward onto the toes at the bottom position, changing the moment arm at the hip and back and creating excessive lower back stress. In lunges and step-ups, the restricted ankle causes the front heel to rise during the drive phase, reducing glute and quad engagement and creating knee stress. In box jumps and plyometrics, restricted ankle dorsiflexion limits the ability to absorb landing forces through the full ankle range, forcing the knee and hip to absorb disproportionate impact — a pattern associated with ACL injury risk in cutting and jumping sports. Even in upper body exercises performed standing, ankle mobility affects stability: insufficient ankle dorsiflexion limits the stable athletic stance width, reducing the base of support during overhead pressing and other standing exercises. This pervasive influence explains why ankle mobility improvements produce such broad performance benefits — it is not merely improving one isolated joint but restoring the foundational mobility that the entire kinetic chain depends on for efficient force transmission.
The Surprising Impact of Ankle Mobility on Upper Body Training
While ankle mobility is most obviously connected to lower body exercises, its influence extends to upper body training through the stability demands of standing exercises. Any exercise performed standing — overhead press, barbell curl, cable exercises — requires a stable base of support from the feet and ankles. Restricted ankle mobility reduces the width of the stable base available for standing exercises by limiting the range in which the ankle can maintain a stable, load-bearing position. This forces a narrower stance or less stable position during standing upper body work, subtly reducing the force production and stability available for the primary exercise. Olympic weightlifters — who must receive heavy barbells overhead in the bottom of a squat position — have consistently among the best ankle dorsiflexion of any athletic population, because the technical requirements of their sport demand it and their training develops it systematically. The lesson for recreational athletes: improving ankle mobility is not merely a lower body training intervention but a whole-body stability improvement that enhances performance across all standing exercises and athletic movements. The foundation of all standing athletic performance is the foot and ankle — developing this foundation through deliberate ankle mobility training produces performance improvements throughout the entire kinetic chain above it.
Why Athletes Ignore Ankle Mobility Until It Is Too Late
The insidious nature of ankle mobility restriction is that it develops gradually — tightening incrementally over months and years until the restriction is severe enough to produce obvious symptoms — and its consequences appear in joints far from the ankle itself. The athlete who develops chronic knee pain from patellar maltracking, or recurring lower back pain during squatting, or persistent Achilles tendinopathy from altered gait mechanics, rarely connects these symptoms to ankle restriction because the ankle itself often feels fine and the symptoms appear elsewhere. This chain of consequences — ankle restriction producing compensations that stress distant joints — means that ankle mobility problems are frequently treated symptomatically at the site of pain (the knee, the back, the hip) while the ankle restriction driving the compensation continues unchallenged. The result is chronic recurrence of symptoms despite treatment, because the mechanical driver of the symptom has not been addressed. Understanding this chain of consequences reframes ankle mobility work from optional enhancement to essential maintenance — the investment that prevents the downstream joint problems that restricted ankle function reliably produces across years of cumulative loading.
The ankle is the foundation of every standing movement — improving its mobility produces the broadest performance transfer of any joint-specific intervention available in physical training.
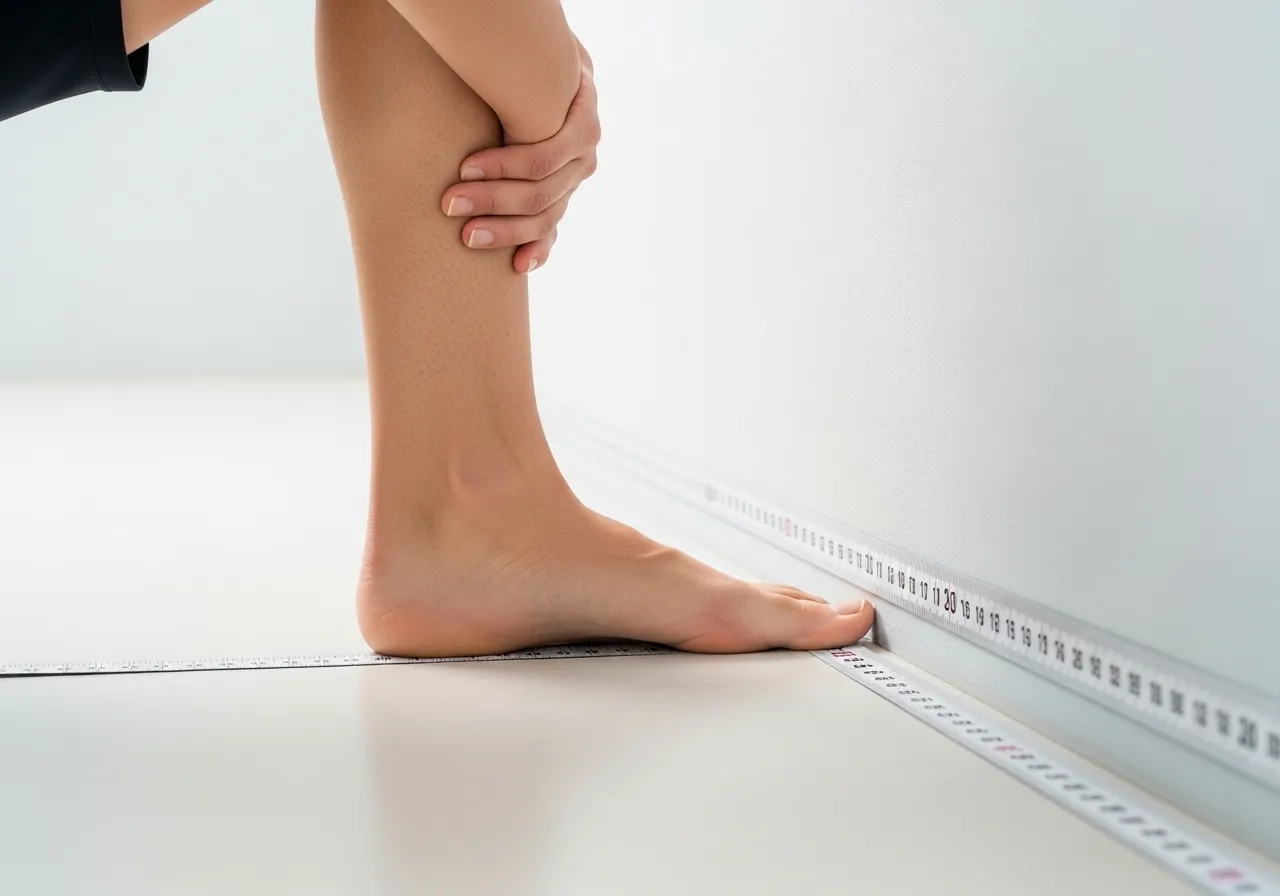
How to Measure Your Ankle Mobility and What the Numbers Mean
The Knee-to-Wall Test
The knee-to-wall test is the most practical and well-validated ankle dorsiflexion assessment available without equipment. Stand facing a wall with one foot parallel to it, toes pointing at the wall. Move the foot back from the wall until the knee can just barely touch the wall while keeping the heel flat on the floor. Measure the distance from the big toe to the wall at this position. A distance of less than 9 to 10cm indicates restricted ankle dorsiflexion that is likely limiting squatting mechanics and running efficiency. A distance of 10 to 13cm represents adequate mobility for most activities. Greater than 13cm represents excellent ankle mobility.
Test both sides and compare. A difference of more than 2cm between sides indicates a unilateral restriction — common after ankle sprains or in people with a dominant-side movement pattern — that requires specific attention to the more restricted side.
The Overhead Squat Assessment
A secondary ankle mobility screen: perform an air squat with arms raised overhead. If the heels rise, the torso falls significantly forward, or you cannot descend to parallel, ankle dorsiflexion restriction is likely the primary cause (though hip mobility and thoracic extension may also contribute). The heels-rising indicator is the most specific to ankle restriction. Performing the same squat with 2cm heel elevation (standing on small plates) and observing whether depth improves confirms that ankle dorsiflexion is the limiting factor — if depth immediately improves with heel elevation, the ankle is restricting your squat, not hip or thoracic limitations.
Interpreting Your Assessment
Knee-to-wall distance under 9cm: significant restriction requiring daily targeted mobility work and possibly assessment by a physiotherapist to rule out structural or post-injury contributions. 9 to 10cm: moderate restriction that daily mobility work reliably improves within 4 to 8 weeks. 10 to 13cm: adequate for most activities but will improve with regular practice, particularly benefiting squat depth and running efficiency. Above 13cm: normal range, maintain with regular use and periodic mobility work.
Differentiating Soft Tissue Restriction From Joint Capsule Restriction
The treatment approach for ankle mobility restriction depends critically on whether the limitation comes from tight muscles and tendons (soft tissue restriction) or from a stiff posterior joint capsule (joint restriction). These two sources feel similar from the outside but respond to different interventions. Soft tissue restriction from the gastrocnemius and soleus responds to stretching — the standard calf stretches that most people know. Joint capsule restriction does not respond to stretching but does respond to joint mobilization — specifically, the banded ankle distraction technique that creates a posterior-to-anterior glide of the talus within the ankle mortise. Identifying which type of restriction is present: if calf stretching produces a clear pulling sensation in the calf and Achilles region, soft tissue restriction is likely the primary cause. If stretching produces minimal calf sensation but the ankle still lacks range, or if there was a history of ankle sprains, joint capsule restriction may be the primary cause. Most people with chronic ankle mobility restriction have both components, requiring both stretching for the soft tissue component and banded mobilization for the joint component. According to Journal of Orthopaedic and Sports Physical Therapy research, banded ankle mobilization produces immediate, clinically meaningful improvements in dorsiflexion range that calf stretching alone cannot achieve in individuals with posterior capsule restriction.
The Frequency Principle in Ankle Mobility Development
Ankle mobility responds to training frequency more than to session duration — ten minutes of ankle mobility work daily produces substantially better outcomes than one hour of ankle mobility work once per week, because the tissues require repeated low-stress exposure to adapt their viscoelastic properties. The mechanism: connective tissue (tendons, joint capsules, fascia) remodels slowly through collagen synthesis and reorientation, a process that requires repeated stimulus signals rather than infrequent intense stretching sessions. Daily ankle mobility practice provides the stimulus frequency that drives connective tissue adaptation; weekly practice provides insufficient signals for the adaptation machinery to prioritize ankle tissue remodeling. The practical application: performing the four-exercise ankle mobility sequence described in this article takes eight to ten minutes. Doing it daily for eight weeks produces dramatically better results than doing it once or twice per week for the same total time. Habit stacking — attaching the ankle mobility routine to an existing daily habit like morning coffee, teeth brushing, or the gym warm-up — dramatically improves adherence to the daily frequency that produces results. Research on stretching frequency and flexibility development confirms that daily stretching produces significantly greater range of motion improvements than equivalent-volume training performed at lower frequencies, validating the daily practice approach for ankle mobility development specifically.
Self-Assessment: The Three-Position Ankle Test
Beyond the standard knee-to-wall test, a three-position assessment reveals more complete information about ankle mobility limitations. Position one: standing calf stretch with knee straight (tests gastrocnemius flexibility). Position two: bent-knee calf stretch (tests soleus flexibility specifically). Position three: weight-bearing deep squat hold at maximum depth (tests integrated ankle mobility under load). Comparing restriction across all three positions identifies the specific limiting structure. Equal restriction in all three positions suggests joint capsule restriction as a significant component. Greater restriction in position one than position two suggests gastrocnemius dominance. Adequate isolated stretching in positions one and two but restriction in position three suggests motor control and stability limitations in addition to flexibility, requiring loaded ankle training rather than passive stretching alone. This differentiated assessment prevents the common error of applying the wrong intervention — stretching when joint mobilization is needed, or passive mobility work when loaded stability training is the actual requirement.
Ankle Mobility and Lower Back Pain: An Underrecognized Connection
Lower back pain during squatting and deadlifting is frequently attributed to lumbar spine mobility or hip mobility limitations, but restricted ankle dorsiflexion is an underrecognized contributor to compensatory lumbar flexion. When the ankle cannot dorsiflex sufficiently during the squatting movement, the tibia cannot advance over the foot, forcing the hips to shoot backward or the torso to lean excessively forward to maintain balance. Both compensations increase the moment arm at the lumbar spine, dramatically increasing the compressive and shear forces on lumbar discs and facet joints. Research using motion capture analysis of squat mechanics finds that improving ankle dorsiflexion by ten degrees reduces peak lumbar flexion during squatting by five to eight degrees — a meaningful reduction in the primary mechanical factor associated with squat-related lumbar disc stress. For people experiencing lower back pain during squatting despite adequate hip mobility and technique coaching, ankle dorsiflexion assessment and treatment should be the next diagnostic step before attributing the problem to the lumbar spine or hip. According to biomechanical research on squat mechanics and lumbar stress, ankle dorsiflexion is one of the primary determinants of lumbar moment arm during deep squatting, confirming the ankle’s critical role in protecting the lower back during loaded squat movements.
The Banded Ankle Distraction Technique: The Most Effective Joint Mobilization
Banded ankle distraction is the most effective technique for addressing posterior ankle capsule restriction — the joint mobility limitation that standard stretching cannot resolve. The setup: loop a thick resistance band around a squat rack post at ankle height, step into the band so it wraps around the front of the ankle just above the foot, and step far enough forward to create significant band tension that pulls the ankle posteriorly. From this position, drive the knee forward over the toe repeatedly for two minutes, then hold the deepest comfortable dorsiflexion position for thirty seconds. The band tension creates a posterior-to-anterior distraction force on the talus within the ankle mortise, mobilizing the posterior capsule that restricts anterior glide of the talus — the joint mechanics required for dorsiflexion. Research from physical therapy confirms that this technique produces immediate, clinically meaningful improvements in dorsiflexion range that persist for twenty-four to forty-eight hours after the session, providing the therapeutic window during which squatting and mobility practice can reinforce the gained range. Performing banded ankle distraction before squatting or other lower body training takes advantage of this therapeutic window by training the movement pattern in the newly available range — the combination that produces lasting rather than temporary mobility improvements. Physical therapists use this technique routinely for post-sprain rehabilitation and for general ankle mobility improvement, validating its effectiveness in clinical populations with diagnosed mobility restrictions as well as in healthy athletes seeking performance enhancement.
Understanding the distinction between these restriction types prevents the frustration of applying the wrong intervention for weeks without result — the athlete who identifies joint capsule restriction and switches from stretching to banded mobilization typically sees the improvement in weeks that stretching alone failed to produce in months.

The Four Best Ankle Mobility Exercises
Exercise 1: Knee-to-Wall Ankle Circles (The Mobility Builder)
Stand facing a wall with one foot approximately 5cm from the wall. Drive the knee forward toward the wall while keeping the heel flat — you should feel the stretch in the anterior ankle and Achilles. Perform small circles with the knee at this maximum dorsiflexion range, 10 circles each direction. Move the foot slightly further from the wall and repeat. This active mobilization technique — moving through the range rather than holding a static stretch — produces faster range of motion improvement than static stretching alone because it trains the joint through active range rather than passively holding at the end range.
Exercise 2: Banded Ankle Mobilization (The Capsule Release)
This exercise specifically addresses posterior ankle capsule restriction — the joint restriction component that calf stretching cannot reach. Loop a resistance band around a sturdy anchor at ankle height. Place the band low around the front of the ankle of the working foot, step forward to create tension in the band pulling the talus (ankle bone) posteriorly, and perform controlled squat descents and ankle circles against the band. The band distraction specifically mobilizes the posterior capsule, releasing the restriction that tighten after ankle sprains and through sedentary patterns. This is the exercise most commonly prescribed by physiotherapists for stubborn ankle mobility restriction — and the one most commonly absent from general fitness programs. Research on ankle mobility interventions confirms that joint mobilization techniques addressing the posterior capsule produce greater dorsiflexion improvements than stretching-only approaches for individuals with significant restriction.
Exercise 3: Deep Squat Hold With Active Ankle Work (The Integration)
Using a squat rack or doorframe for support if needed, descend into the deepest squat position achievable with flat feet. From this position, rock forward and backward slightly — actively pressing the knees further over the toes and then returning — for 20 to 30 repetitions. This active work at the end range of the squat simultaneously stretches the ankle, strengthens the dorsiflexors, and trains the movement pattern that the ankle restriction is limiting. The deep squat hold alone provides a useful stretch; the active movement converts passive stretch into functional mobility improvement that transfers to actual squatting and running.
Exercise 4: Single Leg Calf Raises With Full Range (The Strength Component)
Ankle mobility without the strength to control it is incomplete. Single leg calf raises performed through the complete range — full plantarflexion at the top, full dorsiflexion at the bottom with heel dropping below the step — simultaneously stretch the calf and Achilles at the bottom range and strengthen the calf at the top. Perform 3 sets of 15 with slow eccentrics (3 seconds lowering) on each side. The slow eccentric specifically develops the Achilles tendon’s elastic properties and provides the eccentric calf strength that prevents re-restriction after mobility is achieved. This exercise is the most effective single tool for maintaining ankle mobility improvements over time.
Ankle Mobility and Knee Pain: The Connection Most Lifters Miss
Patellofemoral pain syndrome — the anterior knee pain that plagues runners, cyclists, and squatters — is frequently caused or perpetuated by restricted ankle dorsiflexion rather than by knee-specific dysfunction. When the ankle cannot dorsiflex adequately, the tibial advancement required for squat mechanics is compensated by increased tibial internal rotation, which drives the femur into internal rotation as well — placing the patella in a laterally displaced tracking position that creates compressive stress between the patella and the lateral femoral condyle. This patellar maltracking, driven by ankle restriction, produces the characteristic anterior knee pain of patellofemoral syndrome during any activity requiring knee flexion. The diagnostic test: perform a bodyweight squat with the heels elevated two to three centimeters (simulating improved ankle dorsiflexion). If knee pain is reduced or eliminated with heel elevation, ankle restriction is almost certainly contributing to the knee symptoms. Treatment directed at the ankle through the mobility program described in this article then addresses the source of the knee pain rather than merely managing the symptom at the knee. Physical therapists who specialize in running and lower extremity injuries consistently include ankle dorsiflexion assessment and treatment as a primary component of patellofemoral pain rehabilitation, based on the well-established biomechanical link between ankle restriction and knee tracking dysfunction. Research on ankle dorsiflexion and patellofemoral pain confirms this relationship, finding significantly restricted ankle dorsiflexion in patellofemoral pain patients compared to pain-free controls.
Progressive Ankle Mobility Programming: 12 Weeks to Functional Range
A structured twelve-week ankle mobility program produces meaningful, lasting improvement in dorsiflexion range for most people with moderate restriction. Weeks one to four: daily soft tissue work (two minutes of gastrocnemius stretching with knee straight, two minutes of soleus stretching with knee bent) plus two minutes of knee-to-wall ankle circles per side. Goal: establish the daily habit and begin the gradual tissue adaptation. Weeks five to eight: add banded ankle mobilization (two minutes per side) to address joint capsule restriction alongside the stretching work. Monitor knee-to-wall test distance weekly to confirm progress. Weeks nine to twelve: integrate loaded ankle mobility work — deep squat holds with active ankle dorsiflexion, single-leg calf raises through full range — to develop strength and motor control in the newly available range. Without this loaded integration, mobility gained in isolation does not transfer reliably to movement patterns under load. The twelve-week endpoint is not the end of ankle mobility work but the establishment of a maintenance program — ten minutes of daily ankle mobility practice, reduced from the initial intensive program — that preserves the gained range permanently. Mobility that is not maintained through continued practice is progressively lost as the adaptive tissues return to their original shortened state without the repeated stimulus that produced the improvement. ACSM flexibility training guidelines support regular ongoing flexibility maintenance as necessary for preserving mobility gains achieved through dedicated training programs.
Ankle Mobility and Athletic Power Development
Power athletes — sprinters, jumpers, throwers — require specific ankle stiffness during the ground contact phase of jumping and sprinting to efficiently transfer force from the leg muscles through the ankle and into the ground. This might seem to contradict the emphasis on ankle mobility, but the relationship between mobility and stiffness is complementary rather than contradictory: athletes need adequate dorsiflexion range to achieve optimal joint positions during athletic movements, but they also need the neuromuscular stiffness to control that range under high-speed loading conditions. Ankle mobility work develops the passive range; plyometric training and sprint mechanics develop the neuromuscular stiffness that uses that range efficiently. Athletes who lack sufficient dorsiflexion cannot achieve the optimal joint positions for force transfer regardless of how much neuromuscular stiffness they develop — the ankle mobility is the prerequisite that makes efficient power transfer possible. Research on sprint mechanics and ankle function confirms that elite sprinters have both greater ankle dorsiflexion range and greater ankle joint stiffness during ground contact than recreational runners — demonstrating that mobility and stiffness are developed simultaneously through appropriate training rather than trading off against each other. The ankle mobility program described in this article develops the mobility prerequisite; integrating it with the plyometric and speed work that develops ankle stiffness produces the complete ankle function that athletic performance requires. Research on ankle mechanics and sprint performance confirms the critical role of adequate ankle dorsiflexion in efficient force transmission during ground contact in sprinting and jumping activities.
The four ankle mobility exercises described in this article address all three of the primary restriction sources — gastrocnemius and soleus flexibility, posterior joint capsule mobility, and integrated motor control under load — making them collectively sufficient for most recreational athletes to achieve and maintain functional ankle dorsiflexion across years of training.

Ankle Mobility and Your Squat: Fixing the Root Cause
How Ankle Restriction Changes Your Squat Mechanics
When the ankle reaches its dorsiflexion limit during the squat descent, one of four compensations occurs: the heel rises (most common), the knee tracks inward to allow the shin to remain more vertical, the torso pitches forward to shift the center of mass back over the now-immobile foot, or the squat simply stops short of full depth. Each compensation has downstream consequences: rising heels destabilize the lift and reduce posterior chain loading; knee valgus creates medial knee stress; forward torso lean increases spinal loading and reduces quad activation; limited depth reduces the training stimulus of the squat.
The practical test: perform back squats and front squats with your current mobility and with a 2cm heel elevation (plates under the heels). If the heel-elevated version shows noticeably better depth, upright torso, and knee tracking, ankle mobility is the primary limiting factor in your squat. Fixing the ankle changes the squat completely.
Short-Term vs Long-Term Solutions
Short term: use heel elevation (weightlifting shoes, heel wedges, or plates under the heels) to compensate for current ankle restriction while training the squat productively. This allows full-range squatting immediately while ankle mobility develops. Long term: the ankle mobility exercises in the previous section, performed daily for 8 to 12 weeks, produce the structural changes that eliminate the need for heel elevation. Combining the short-term accommodation with the long-term fix produces the best outcome: continued productive training alongside systematic mobility development.
Monitoring Squat Improvement from Ankle Mobility Work
Retest the knee-to-wall distance every three weeks to track progress. Most people with moderate restriction (9 to 11cm baseline) achieve adequate mobility (12 to 13cm) within 6 to 10 weeks of daily mobility work. The squat improvement from this mobility gain is typically dramatic — lifters who have squatted with heel elevation for years often experience significant depth and position improvement when ankle mobility finally allows flat-foot squatting with good mechanics.
Ankle Mobility for Running: Stride Length, Efficiency, and Injury Prevention
Running mechanics depend on ankle dorsiflexion at the moment of initial contact — the ankle must dorsiflex as the foot lands and the tibia advances over the foot during the stance phase. Restricted dorsiflexion at this moment creates two compensatory patterns: overstriding (landing with the foot further in front of the center of mass, creating a braking force that increases impact and reduces efficiency) or excessive pronation (the ankle rolling inward to create apparent dorsiflexion through foot mechanics rather than true ankle range of motion). Both compensations increase injury risk — overstriding is associated with anterior shin pain and stress fractures; excessive pronation is associated with plantar fasciitis, Achilles tendinopathy, and medial knee stress. Research quantifying the relationship between ankle dorsiflexion and running injury finds that less than 35-36 degrees of weight-bearing ankle dorsiflexion increases injury risk by two to three times in runners — a highly significant threshold that many recreational runners fall below without realizing it. The knee-to-wall test approximates this threshold: the ability to touch the knee to a wall with the foot 10-12 centimeters from the wall while keeping the heel flat corresponds roughly to adequate dorsiflexion for running mechanics. Improving from below this threshold to above it through the ankle mobility program described in this article produces measurable stride length improvements, running economy improvements of three to five percent, and significant reduction in the overuse injury patterns caused by restricted dorsiflexion. Research on ankle dorsiflexion and running injury risk confirms this relationship across multiple study populations of recreational and competitive runners.
Ankle Mobility Testing Standards: What Normal Looks Like
Establishing normative standards for ankle dorsiflexion provides a target for the mobility program and context for interpreting individual assessment results. The weight-bearing knee-to-wall test normative values: reaching the wall with the foot 10-12 centimeters from the wall is considered functional; 13-15 centimeters indicates good dorsiflexion; above 15 centimeters indicates excellent mobility. Values below 10 centimeters indicate meaningful restriction that likely affects squat mechanics, running efficiency, or both. Non-weight-bearing dorsiflexion (measured lying down with a goniometer) normative values are 20 degrees minimum for basic function, with 20-30 degrees considered normal range and above 30 degrees indicating above-average mobility. The discrepancy between weight-bearing and non-weight-bearing measurements is diagnostically useful — a large discrepancy (good non-weight-bearing range but poor weight-bearing range) suggests joint capsule restriction rather than muscle tightness, because the joint capsule is loaded under body weight in ways that are not replicated in the non-weight-bearing position. Tracking knee-to-wall test distance monthly through the twelve-week program provides objective measurement of the improvement being produced, keeping training targeted and motivated through periods when the improvement is happening at the tissue level but not yet clearly perceivable in daily movement.
Ankle Mobility in Specific Sports: Basketball, Soccer, and Weightlifting
Different sports create different ankle mobility demands and different ankle mobility limitations. Basketball players require exceptional ankle dorsiflexion for the deep squat positions of defensive stance and landing from jumps, plus lateral ankle stability for the rapid direction changes that characterize the sport. The combination of frequent ankle sprains from landing and cutting movements and the specific dorsiflexion demands of the sport makes ankle mobility a primary performance and injury prevention focus for serious basketball players. Soccer players face similar ankle demands for shooting mechanics (optimal ankle position for ball contact), jumping for headers (landing mechanics), and the rapid acceleration-deceleration of attack and defense. Olympic weightlifters require the greatest ankle dorsiflexion of any athletic population — receiving a snatch or clean in the bottom position with a barbell overhead requires dorsiflexion exceeding 40-45 degrees in many athletes, far beyond the 20-30 degree norms of the general population. Weightlifters achieve this through years of specific ankle mobility work and the adaptive demands of their training, and their ankle mobility development approaches are increasingly being adopted by general fitness athletes for the comprehensive ankle range they produce. Swimmers paradoxically develop ankle plantarflexion (pointing the foot) rather than dorsiflexion from their sport — elite swimmers have exceptional plantarflexion for the flutter kick but often have restricted dorsiflexion that limits land-based squatting and jumping mechanics, making ankle dorsiflexion work specifically important for swimmers who also perform land-based training. Research on sport-specific ankle mobility demands confirms that different sports create different ankle mobility profiles and that training programs should account for sport-specific ankle demands when prescribing mobility work.
Using Video Analysis to Monitor Ankle Mobility Progress in Squatting
Video analysis provides objective feedback on ankle mobility improvement that subjective perception cannot reliably deliver. Filming the squat from the side, with clear visibility of the heel, ankle, and knee, reveals whether the heel remains planted throughout the movement, whether the tibia advances appropriately over the foot, and whether the knee tracks in alignment with the toe or caves inward — the compensation pattern most commonly associated with ankle restriction. Monthly video comparisons, filmed from the same angle and at the same squat depth, document the mechanical improvements that accompany ankle dorsiflexion development: the heel remaining planted to greater depths over weeks, the shin angle becoming more vertical (indicating better dorsiflexion utilization), and the knee tracking improving as the ankle restriction that drove valgus compensation resolves. This video documentation serves two purposes: it provides objective evidence of improvement during periods when subjective perception cannot detect the gradual changes occurring, and it reveals whether ankle mobility improvements are translating into improved squat mechanics or whether other movement limitations are now the limiting factor requiring attention. The comprehensive movement assessment that video analysis enables transforms ankle mobility training from a hopeful intervention into a data-driven process with clear outcome measurement.
The squat mechanics improvements that follow consistent ankle mobility work are among the most dramatic technique transformations available through a single intervention — athletes who previously needed significant heel elevation to squat comfortably often reach full depth flat-footed within eight to twelve weeks of dedicated ankle dorsiflexion development, fundamentally changing the quality and muscle engagement of their most important lower body exercise.

Ankle Mobility for Runners: Why Every Stride Depends on This
Running Mechanics and Ankle Dorsiflexion
Every running stride requires the ankle to dorsiflex during the stance phase — the period when the foot is on the ground and the body is moving forward over it. Restricted dorsiflexion during running forces compensatory mechanics: the foot pronates excessively inward to achieve ground clearance, the hip externally rotates to compensate, and the knee experiences elevated medial stress from the altered ground contact pattern. These compensatory mechanics are among the primary causes of the most common running injuries: medial tibial stress syndrome (shin splints), patellofemoral pain syndrome (runner’s knee), plantar fasciitis, and Achilles tendinopathy.
Research on running biomechanics and ankle mobility finds a direct correlation between restricted ankle dorsiflexion and injury rates in runners. Research on ankle dorsiflexion and running injury risk confirms that restricted ankle dorsiflexion is a measurable risk factor for lower extremity running injuries, and that dorsiflexion improvement reduces injury incidence in runners across training levels.
The Daily Ankle Routine for Runners
For runners specifically: perform the four exercises above daily, with particular emphasis on the banded ankle mobilization and the single-leg calf raise. Add walking lunges with deliberate forward knee drive over the toes as a warm-up before running sessions — this active dorsiflexion through the gait pattern prepares the ankle for running mechanics. Most runners with moderate dorsiflexion restriction who complete 6 weeks of daily ankle mobility work report noticeable reductions in shin tightness, improved push-off sensation, and reduced anterior knee discomfort during and after runs.
Frequently Asked Questions About Ankle Mobility
How long will it take to improve my ankle mobility? Most people with moderate restriction (knee-to-wall distance under 10cm) achieve meaningful improvement within 4 to 6 weeks of daily mobility work. Significant structural restriction from previous ankle sprains or long-standing limitation may require 8 to 12 weeks. The banded ankle mobilization produces faster improvement than stretching alone for capsule-restricted ankles. Daily practice is more important than session length — 5 minutes daily produces faster improvement than 30 minutes twice weekly.
Should I get orthotics if my ankle mobility is restricted? Orthotics address the symptoms of ankle restriction — altered foot mechanics — without improving the restriction itself. They may be appropriate for managing pain while mobility improves, but they are not a substitute for mobility work. A physiotherapist specializing in running or lower extremity biomechanics can advise on whether orthotics are appropriate for your specific presentation alongside mobility training.
My ankle mobility is good but I still have squat problems. What else could it be? Hip mobility (particularly internal rotation and flexion) and thoracic extension are the other most common squat limitation causes. If ankle mobility tests normal (above 12cm knee-to-wall) but squat mechanics are still compromised, assess hip mobility and thoracic extension as the next investigation areas. A single movement assessment session with a qualified coach or physiotherapist typically identifies the specific limiting factor more efficiently than self-directed investigation. NSCA resources on mobility and movement screening provide validated assessment tools for identifying movement limitations in resistance training.
Is it too late to improve ankle mobility if I am over 40? No — ankle mobility responds to targeted training at any age. The rate of improvement may be somewhat slower due to reduced tissue elasticity, but the direction of change is the same. Adults over 40 with significant ankle restriction commonly see substantial improvement within 8 to 12 weeks of consistent daily mobility work. The functional benefits — better squat mechanics, reduced joint stress, improved balance and proprioception — are particularly valuable for older adults because they directly support the movement quality that functional independence requires.
Ankle Mobility Exercises Beyond the Basics: Advanced Applications
Once basic ankle dorsiflexion is established through the foundational four exercises, more advanced ankle mobility and stability work develops the full ankle function required for high-level athletic performance. Single-leg ankle stability exercises — standing on one leg while tracing the alphabet with the opposite foot — develop the proprioceptive and neuromuscular control that turns passive range of motion into active stability under load. Eccentric calf lowering — standing on a step edge and slowly lowering the heel below the step level — develops the Achilles tendon strength and ankle dorsiflexion range simultaneously, addressing both the flexibility and strength components of ankle function that stretching alone cannot develop. Lateral ankle stability exercises — mini-band lateral walks and single-leg balance on unstable surfaces — develop the peroneal muscles that control lateral ankle stability and prevent the inversion sprains that are the most common athletic ankle injury. Integrating these advanced exercises into a comprehensive ankle program after the basic mobility foundation is established produces the full ankle function — mobility, stability, strength, and proprioception — that athletic performance requires. Athletes who complete this progressive ankle development consistently report improvements not just in the specific exercises that ankle mobility targeted but in running efficiency, jumping mechanics, and the general sense of athleticism that adequate ankle function enables across all movement patterns.
Footwear and Its Effect on Ankle Mobility
Modern athletic footwear — particularly running shoes with significant heel-to-toe drop — chronically shortens the gastrocnemius and soleus by maintaining the ankle in slight plantarflexion throughout the day. The accumulated effect of twelve to sixteen hours daily of heel-elevated foot positioning is progressive soft tissue shortening that reduces passive ankle dorsiflexion over months and years. This explains the consistent finding that populations who wear minimal footwear or go barefoot throughout their lives have substantially greater ankle dorsiflexion than Western populations who wear conventional athletic footwear from childhood. The practical implication is not necessarily to abandon conventional footwear, but to understand that it creates a mobility challenge that requires active counterbalancing — the ankle mobility program described in this article is essentially counteracting the effect of modern footwear on ankle tissue length. Spending time in minimal footwear or barefoot on appropriate surfaces (home floors, grass, sand) provides passive ankle mobility maintenance by allowing the ankle to move through its natural range during walking rather than maintaining the slightly plantarflexed position that heeled footwear creates. Transitioning to lower-drop footwear should be done gradually over eight to twelve weeks to prevent the Achilles tendon overload that rapid footwear changes produce, as the Achilles must suddenly bear greater eccentric load when heel elevation is reduced.
Maintaining Ankle Mobility Gains Long-Term
Ankle mobility gains achieved through a dedicated training program are not permanent without continued maintenance practice. Connective tissue — tendons, joint capsules, fascia — adapts to the mechanical demands placed on it and reverts toward its previous state when those demands are removed. Athletes who complete an intensive ankle mobility program and then discontinue all ankle-specific work typically lose a significant portion of their gained range within four to eight weeks, as the tissue adaptation reverses in the absence of the continued stimulus that produced it. Maintaining gains requires a maintenance program that is less time-intensive than the initial development program but sufficient to provide the continuing stimulus that prevents regression. A practical maintenance program after achieving functional ankle dorsiflexion: five minutes of ankle mobility work before each lower body training session (knee-to-wall circles and one banded mobilization set per side), plus brief ankle stretching on two non-training days per week. This minimal maintenance dose preserves the gains produced by the initial intensive program while adding minimal time to an established training routine. Athletes who resist maintenance work because they feel the mobility issue is “fixed” consistently rediscover the limitation months later when reduced training frequency allows regression — the lesson, learned with some frustration, that mobility requires ongoing maintenance as reliably as strength requires ongoing training to preserve.
The athlete who commits to daily ankle mobility practice for twelve weeks and progresses through the foundational to advanced exercises consistently emerges with ankle function that transforms their training across all modalities — squatting deeper with better mechanics, running with greater efficiency, and moving through daily life with the ease that adequate ankle dorsiflexion enables. This foundation, once built, requires only maintenance to preserve indefinitely.
Building Ankle Strength Alongside Mobility
Ankle mobility without ankle strength is incomplete — the range of motion must be controllable under load to provide genuine functional benefit. The calf complex (gastrocnemius and soleus) is the primary ankle strength driver, and its strength through the full ankle dorsiflexion range is what determines whether mobility gains translate into improved performance or remain isolated to passive stretching contexts. Single-leg calf raises performed through full available range — starting from maximum dorsiflexion at the bottom and pressing to maximum plantarflexion at the top — develop the strength through the complete range of motion that maximizes the functional value of mobility improvements. Eccentric-only calf lowering (lowering from full plantarflexion to maximum dorsiflexion slowly, using both legs to return to start) specifically develops the eccentric strength that controls ankle dorsiflexion during landing and deceleration — the most injury-prone ankle movements in athletic activity. According to research on eccentric calf training and Achilles tendon health, eccentric calf strengthening through full range significantly reduces Achilles tendinopathy recurrence and improves ankle function in both symptomatic and asymptomatic athletic populations. Integrating this strength work into the ankle mobility program from week four onward ensures that the mobility development is accompanied by the strength development that makes it functionally useful.

Frequently Asked Questions About Ankle Mobility
How long does it take to improve ankle dorsiflexion significantly?
Most people with moderate ankle restriction notice meaningful improvement within four to six weeks of daily ankle mobility practice — the knee-to-wall test distance typically improves two to four centimeters within this timeframe. Reaching functional ankle dorsiflexion standards from a restricted starting point requires eight to twelve weeks of consistent daily practice. Severe restriction from chronic tightness, old injuries, or structural factors may require four to six months of consistent work before reaching functional standards. The rate of improvement depends on the cause of restriction — muscle tightness responds faster than joint capsule restriction, which in turn responds faster than structural bony abnormalities that limit range regardless of soft tissue flexibility. Daily practice is the most important factor in the improvement rate — the difference between daily practice and three-times-per-week practice is not the amount of time spent but the stimulus frequency that drives connective tissue remodeling. NSCA flexibility development guidelines support daily practice as producing two to three times faster range of motion improvement than equivalent-volume less-frequent practice for connective tissue restrictions.
Should I use heel elevation as a permanent solution for ankle restriction?
Heel elevation — using weight plates, wedges, or heel-elevated shoes during squatting — is an appropriate short-term solution that allows productive squatting while ankle mobility is being developed, but should not be used as a permanent substitute for addressing the underlying restriction. Permanent heel elevation does not resolve the ankle mobility limitation and may perpetuate it by maintaining the ankle in a position that reduces the stretch stimulus needed for improvement. The appropriate approach: use heel elevation as needed during training to maintain productive squatting while simultaneously implementing the daily ankle mobility program. As ankle dorsiflexion improves over weeks and months, progressively reduce heel elevation — lowering from two centimeters to one centimeter to flat as the movement pattern accommodates the improved range. This progression bridges the gap between current restriction and functional mobility without sacrificing training productivity during the development period. Most athletes who implement this combined approach — heel elevation for immediate training function plus daily mobility work for long-term resolution — reach unrestricted squatting within eight to sixteen weeks, after which heel elevation becomes unnecessary.
Can old ankle sprains permanently limit dorsiflexion?
Previous ankle sprains frequently cause lasting dorsiflexion restriction through two mechanisms: scar tissue formation in the lateral ligaments that alters joint mechanics, and posterior ankle capsule restriction that develops from the immobility and protective muscle guarding following the injury. These post-sprain restrictions are addressable but require specific joint mobilization techniques (banded distraction) in addition to standard stretching — stretching alone does not adequately address the capsular restriction component. Many people with a history of ankle sprains have never received treatment for the resulting dorsiflexion restriction and experience it as a permanent limitation when it is actually a treatable mobility deficit. Sports physical therapists who specialize in ankle rehabilitation can assess and treat post-sprain dorsiflexion restriction through manual therapy and prescribed home exercises, often producing dramatic range improvements within four to eight weeks of targeted treatment. If ankle mobility self-treatment does not produce clear improvement within four to six weeks despite consistent practice, professional evaluation from a sports physical therapist is warranted to assess whether post-sprain joint mechanics are requiring treatment beyond what self-directed mobility work can provide.
Ankle mobility is one of those rare training investments that pays dividends across virtually every physical activity — improving it makes squatting deeper, running more efficient, jumping higher, and daily movement more comfortable. The ten minutes per day required to develop and maintain it represents one of the highest return-on-investment training practices available, particularly for anyone whose physical activities involve any form of squatting, running, or jumping. Start the assessment today, implement the program tomorrow, and experience the compounding benefits across months of consistent practice.
Every squat, every run, every jump performed with adequate ankle dorsiflexion is a squat, run, or jump performed with better mechanics, greater muscle engagement, and lower injury risk than the same movement performed with restricted ankle function. This cumulative mechanical advantage, compounding across thousands of training repetitions, produces the dramatic performance and health differences between those who address ankle mobility and those who do not.
The cumulative effect of daily ankle mobility work — measured across weeks and months rather than individual sessions — produces the joint health and functional range that protects every lower body exercise and athletic movement for years of continued training.

Integrating Ankle Mobility Work Into Your Current Training Program
Adding ankle mobility work to an existing training program requires minimal time investment when integrated intelligently rather than treated as a separate training session. The most effective integration approach: perform two to three minutes of ankle mobility work as the first component of every lower body training session warm-up, before any other warm-up exercises. This placement ensures the ankle is prepared for the squatting, lunging, and hinging movements that follow, and means the ankle mobility work happens with certainty rather than being relegated to optional post-training work that is frequently skipped when time is limited. On non-training days, a five-minute standalone ankle mobility sequence — knee-to-wall circles and banded mobilization — performed while watching television or during another passive activity requires almost no additional time from the daily schedule. The combination of pre-training ankle mobility during training days and brief standalone sessions on rest days provides the daily stimulus frequency that drives meaningful improvement without requiring dedicated training time beyond what the warm-up already provides. Athletes who resist adding ankle mobility work because they do not have time consistently find that integrating it into existing warm-up routines adds less than three minutes to sessions they were already performing — a trivial time investment relative to the movement quality improvements that follow. According to ACSM warm-up and flexibility guidelines, incorporating flexibility work into training warm-ups is as effective as standalone flexibility sessions for producing range of motion improvements when performed with adequate frequency and duration.
Ankle mobility is the foundation that most athletes overlook until a limitation becomes symptomatic enough to demand attention. Addressing it proactively — through the daily mobility practice, targeted exercises, and progressive loading described in this article — prevents the downstream consequences that restricted ankle dorsiflexion inevitably produces and develops the functional foundation that supports improved performance across all movement patterns for years of continued training.
The Long-Term View: Ankle Mobility as a Lifelong Practice
Ankle mobility, like all physical qualities, requires ongoing maintenance to preserve across the decades of an active life. The good news is that maintenance requires significantly less effort than development — ten minutes of daily mobility work preserves gains that took months of more intensive practice to achieve. Athletes who build excellent ankle mobility in their twenties and maintain it through consistent practice retain dramatically better ankle function into their fifties and sixties than those who do not address ankle mobility until age-related restriction becomes symptomatic. The cumulative difference in movement quality, injury history, and physical capability between those who maintain ankle mobility and those who do not becomes dramatically apparent over decades. Beginning ankle mobility practice at any age produces benefits — it is never too late to improve ankle function — but beginning early and maintaining consistently produces the most comprehensive lifelong benefits. Treating ankle mobility work as a permanent fixture of the training routine rather than a temporary rehabilitation protocol produces the sustained ankle health that supports lifelong athletic practice.
Ankle mobility is the single joint intervention with the broadest performance transfer of any mobility practice — improving it benefits squatting, running, jumping, and daily movement simultaneously. The daily ten-minute commitment that develops and maintains this mobility foundation represents one of the most efficient training investments available to any athlete.












